➤ Someone recently reached out with this message, and it perfectly captures what so many, including myself, have experienced but can't explain:
"I consistently get 6-7 hours of sleep and wake up feeling 'fine,' but I'm not really alert until after coffee. My energy dips, but then I hit the gym and get another wind. Lately though, I need more caffeine and stimulation to maintain focus as the day goes on, and I'm starting to get afternoon crashes. I've been trying to get more sleep but I can't seem to... what's going on?"
They'd tried all the standard sleep optimization advice.
Earlier bedtime, no screens, perfect temperature.
Still felt the same: functional but never truly ‘energized.’
The Problem with Feeling 'Fine' on Less Sleep
This person was describing something I knew intimately. For years, I'd followed the same logic—if I could get through my day after 5-6 hours of sleep, I assumed I was fine.
What we both missed is that our bodies had learned to compensate.
Sleep debt triggers metabolic changes that maintain alertness—increased glucose availability, elevated heart rate. You feel 'fine' because your body is working overtime to compensate.
The problem: while you feel 'fine' from this compensation, something else is happening that most people never connect to their sleep struggles.
The Inflammation Loop: How Poor Sleep Creates An Evil Cycle
Here's where the science gets interesting: inadequate sleep doesn't just make you tired—it triggers a cascade that makes future sleep progressively worse.
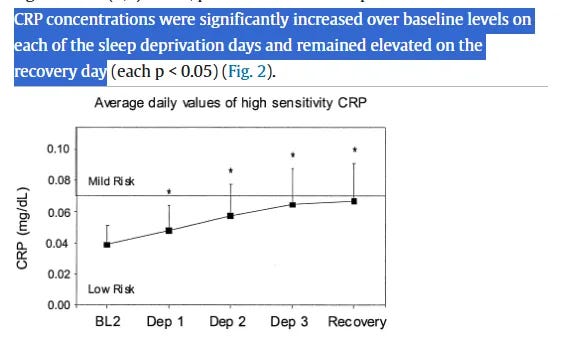
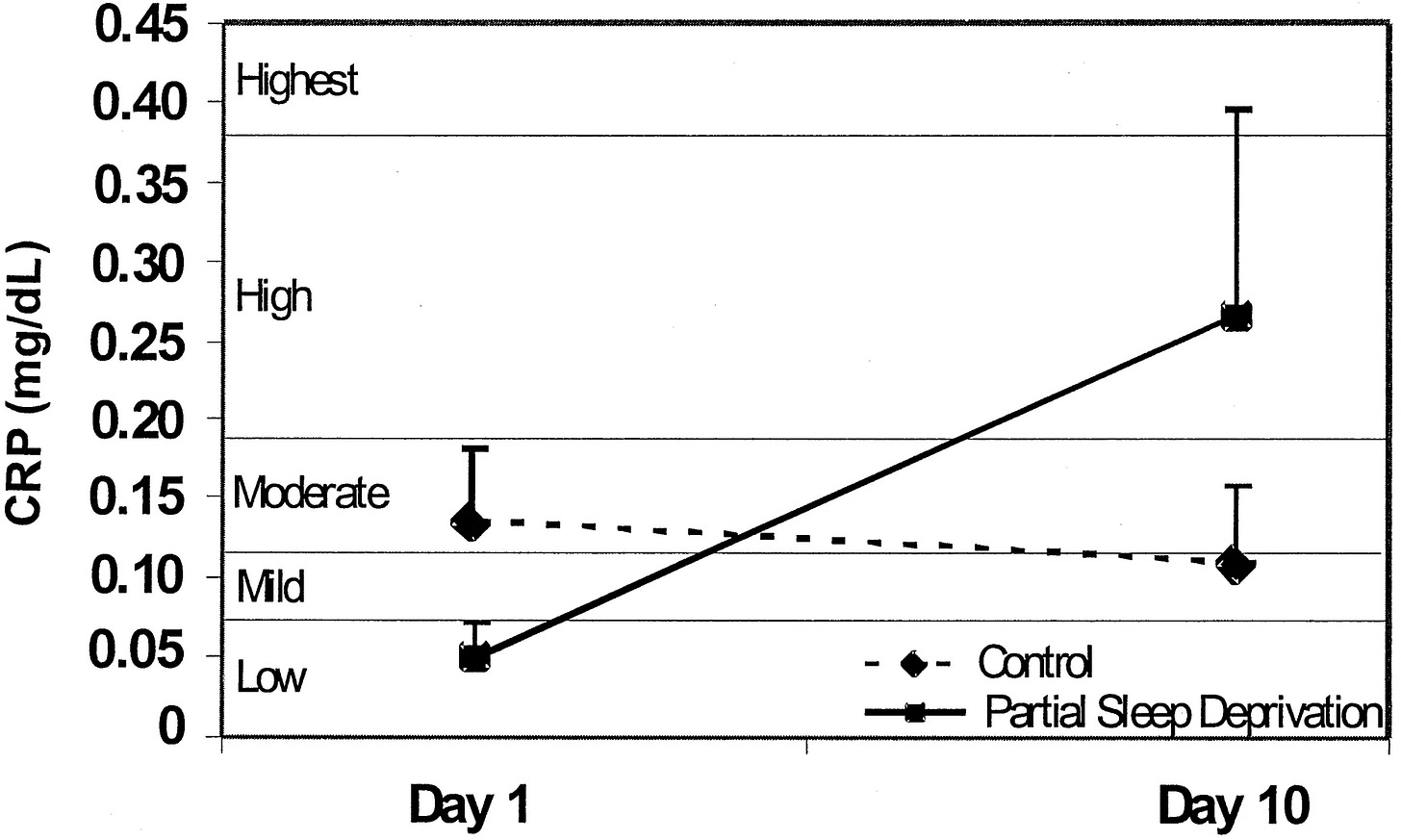
Even mild sleep restriction elevates inflammatory markers like IL-6, TNF-alpha, and C-reactive protein. These inflammatory compounds then disrupt sleep architecture itself, reducing the duration and quality of deep sleep phases where restoration occurs.
This impairs the glymphatic system—your brain's waste clearance mechanism that operates primarily during deep sleep. When this system underperforms, metabolic waste accumulates in neural tissue, contributing to accelerated brain aging and further sleep disruption.
The result: each poor night makes the next one worse.
Sleep debt compounds with interest, creating a self-perpetuating cycle where inflammation disrupts the very neural circuits responsible for sleep regulation.
Research suggests this inflammatory pattern can persist beyond the initial sleep disruption, which may explain why some people struggle with sleep quality even after addressing obvious lifestyle factors.
What Great Sleep Actually Feels Like: What I Learned After 10+ Years Of Sleep Struggles (& another 5+ years to get to 8+ hours a night)
The difference between compensation-driven alertness and genuine restoration became clear when I prioritized sleep architecture over just duration.
The changes were dramatic:
➤ Calmer, more sustained focus—not just bursts of productivity
➤ Easier recovery from workouts, travel, and stress
➤ Better emotional regulation and decision-making
➤ No more afternoon crashes or needing to "push through"
Most importantly: I stopped confusing the wired feeling of caffeine with actual energy.
Real restoration feels steady, not reactive.
Calm.
Focused.
Stoic without trying.
Before experiencing this, I had no idea what I was missing. And I think that's the real problem—
Many of us have normalized how we feel after poor sleep. We've adapted to low energy so well that we've forgotten what fully restored feels like.
There's a difference between being "awake" and being deeply well-rested. Between being alert because you're stressed and alert because your system is truly restored.
It made me rethink that common sleep advice: "if you feel fine during the day, you're probably getting enough."
Because many of us don't realize how underslept we are—we've just adapted to running on borrowed energy.
If you've never experienced deep, consistent, high-quality sleep, you might not know what you're missing.
I didn't.
And now I'll never go back.
Kat
References
Mullington JM, Simpson NS, Meier-Ewert HK, Haack M. Sleep loss and inflammation. Best Pract Res Clin Endocrinol Metab. 2010 Oct;24(5):775-84.
Meier-Ewert HK, Ridker PM, Rifai N, Regan MM, Price NJ, Dinges DF, Mullington JM. Effect of sleep loss on C-reactive protein, an inflammatory marker of cardiovascular risk. J Am Coll Cardiol. 2004 Feb 18;43(4):678-83.
Engert, L.C., Besedovsky, L. Sleep and inflammation: a bidirectional relationship. Somnologie 29, 3–9 (2025).
Irwin MR. Sleep disruption induces activation of inflammation and heightens risk for infectious disease: Role of impairments in thermoregulation and elevated ambient temperature. Temperature (Austin). 2022 Aug 21;10(2):198-234.